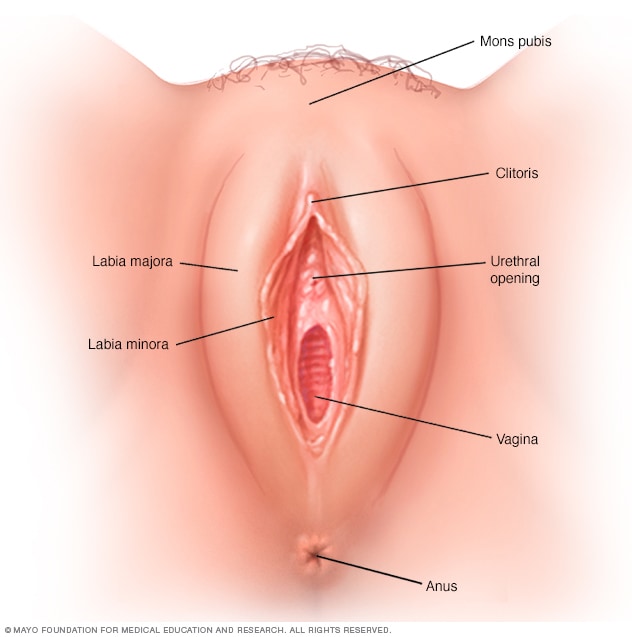
Vagina is the muscular, elastic canal that extends from the vulva to the cervix, serving as the birth canal during delivery, the receptive organ during sexual intercourse, and the outlet for menstrual flow. The vagina is a self-cleaning, pH-regulated environment with complex anatomy involving layered muscular walls, specialized epithelium, and a diverse microbiome that maintains vaginal health through natural defense mechanisms. At the population level, vaginal anatomy shows individual variation in size, shape, and characteristics, with normal vaginal length ranging from 3-6 inches when not aroused, expanding significantly during sexual arousal to accommodate penetration and facilitate reproductive functions.
Vagina | |
|---|---|
| Category | Women’s Health, Reproductive Anatomy, Gynecology |
| Research Fields | Gynecology, Sexual Medicine, Microbiology, Women’s Health |
| Also known as: | Birth canal, vaginal canal, reproductive tract |
| Pronunciation: | vuh-JY-nuh |
| Average length: | 3-6 inches (7.6-15.2 cm) non-aroused |
| Normal pH range: | 3.8-4.5 (acidic) |
| Dominant bacteria: | Lactobacillus species (healthy microbiome) |
| Wall thickness: | 2-3 mm when relaxed |
| Expansion capacity: | 200-300% increase during arousal |
| Sources: | ACOG, Nature Reviews Microbiology, StatPearls, Journal of Sexual Medicine |
The vaginal environment maintains a naturally acidic pH of 3.8-4.5 through the action of beneficial Lactobacillus bacteria, which produce lactic acid and hydrogen peroxide that protect against harmful pathogens. Research demonstrates that the vagina has remarkable adaptive capabilities, with the ability to expand to 200-300% of its resting size during sexual arousal through a process called “tenting,” while vaginal lubrication increases dramatically to facilitate sexual activity and reduce friction-related trauma.
Vaginal health is influenced by numerous factors including hormonal fluctuations throughout the menstrual cycle and lifespan, sexual activity patterns, hygiene practices, medication use, and overall health status. Comprehensive vaginal health awareness encompasses knowledge of normal anatomy and physiology, recognizing signs of health and dysfunction, understanding the importance of the vaginal microbiome, and evidence-based approaches to maintaining optimal vaginal wellness throughout life.
History
Ancient Understanding
Ancient civilizations documented basic knowledge of female reproductive anatomy, though understanding was often limited by cultural taboos and anatomical study restrictions. Egyptian, Greek, and Roman medical texts included references to vaginal anatomy and associated health conditions, though interpretations were frequently influenced by prevailing beliefs about women’s bodies.
Medieval and Renaissance Anatomical Study
Medieval medical knowledge about vaginal anatomy was largely based on ancient texts and limited direct observation. The Renaissance period brought renewed interest in anatomical study, with anatomists like Andreas Vesalius beginning more systematic documentation of female reproductive anatomy, though cultural constraints still limited detailed investigation.
18th-19th Century: Scientific Development
The development of more systematic medical education and anatomical study during this period led to improved understanding of vaginal structure and function. Early gynecological texts began documenting normal variations and pathological conditions, laying groundwork for modern gynecological practice.
Early 20th Century: Hormonal Discoveries
The discovery of reproductive hormones and their effects on vaginal tissues revolutionized understanding of how hormonal fluctuations influence vaginal health throughout the menstrual cycle, pregnancy, and menopause. This knowledge enabled better treatment of hormonal disorders affecting vaginal function.
Mid-20th Century: Sexual Health Research
Pioneering research by scientists like Masters and Johnson provided detailed physiological understanding of vaginal changes during sexual arousal and response. This research helped establish normal sexual function parameters and identify pathological conditions affecting sexual health.
1980s-1990s: Microbiome Recognition
Advanced microbiological techniques revealed the complex ecosystem of vaginal microorganisms and their role in maintaining health. Understanding of bacterial vaginosis, yeast infections, and the protective role of Lactobacillus species transformed approaches to diagnosing and treating vaginal infections.
2000s-Present: Molecular and Genomic Research
Modern molecular techniques have enabled detailed characterization of the vaginal microbiome, hormonal regulation of vaginal tissues, and genetic factors influencing vaginal health. Contemporary research continues advancing understanding of vaginal immunology, sexual function, and personalized approaches to vaginal health management.
Anatomy and Structure
Basic Anatomical Structure
The vagina is a fibromuscular tube extending from the vulva to the cervix, positioned between the bladder anteriorly and the rectum posteriorly. The vaginal canal is normally collapsed with its walls touching, creating a potential space that can expand significantly when needed for sexual activity, medical examination, or childbirth.
Vaginal Walls and Layers
The vaginal wall consists of three layers: the inner mucosa (epithelium), the middle muscularis (smooth muscle), and the outer adventitia (connective tissue). The mucosa has characteristic rugae (folds) that allow for expansion, while the muscular layer provides contractile capability and structural support.
Anatomical Relationships
The vagina is surrounded by important anatomical structures including the pelvic floor muscles, urethral and bladder tissues, rectal wall, and pelvic blood vessels and nerves. Understanding these relationships is crucial for medical procedures and recognizing how conditions affecting adjacent structures may impact vaginal health.
Individual Anatomical Variation
Normal vaginal anatomy shows considerable individual variation in length, width, angle, and internal structure. These variations are normal and don’t typically affect function, though they may influence comfort with certain sexual positions, tampon use, or medical procedures.
Physiological Functions
Reproductive Functions
The vagina serves as the receptive organ during sexual intercourse, allowing sperm to reach the cervix and potentially fertilize eggs. During childbirth, the vagina acts as the birth canal, expanding dramatically to allow fetal passage while protecting surrounding structures through its elastic properties.
Menstrual Function
The vagina provides the outlet for menstrual flow, with the vaginal environment adapting to accommodate regular monthly discharge of endometrial tissue and blood. Normal menstrual flow patterns help maintain vaginal health through regular flushing of the vaginal canal.
Self-Cleaning Mechanisms
The vagina is naturally self-cleaning through several mechanisms including normal vaginal discharge that carries away dead cells and potential pathogens, the acidic environment that inhibits harmful bacterial growth, and the action of beneficial bacteria that compete with and suppress pathogenic organisms.
Sexual Response
During sexual arousal, the vagina undergoes dramatic physiological changes including increased blood flow, vaginal tenting (elongation and expansion), increased lubrication production, and enhanced sensitivity. These changes facilitate sexual activity and optimize conditions for potential conception.
Vaginal Microbiome
Normal Bacterial Flora
A healthy vaginal microbiome is typically dominated by Lactobacillus species, which produce lactic acid and hydrogen peroxide that maintain the acidic vaginal environment. The most common species include L. crispatus, L. gasseri, L. iners, and L. jensenii, though composition varies among individuals and populations.
Microbiome Functions
The vaginal microbiome protects against infections by maintaining acidic pH, producing antimicrobial compounds, competing with pathogens for nutrients and attachment sites, and supporting local immune function. Vaginal microbiome research continues revealing complex interactions between bacteria, immune function, and overall health.
Factors Affecting Microbiome
The vaginal microbiome is influenced by hormonal fluctuations, sexual activity, antibiotic use, hygiene practices, stress levels, diet, and genetic factors. Understanding these influences helps explain why some women are more susceptible to vaginal infections and guides preventive strategies.
Microbiome Disruption
Disruption of the normal vaginal microbiome can lead to conditions like bacterial vaginosis, yeast infections, or increased susceptibility to sexually transmitted infections. Restoration of healthy microbiome balance is often a key component of treating vaginal health problems.
Hormonal Influences
Estrogen Effects
Estrogen is the primary hormone affecting vaginal health, promoting vaginal epithelial thickness, maintaining elasticity, supporting lubrication production, and helping sustain the acidic environment. Adequate estrogen levels are essential for optimal vaginal structure and function.
Menstrual Cycle Changes
The vagina undergoes cyclical changes throughout the menstrual cycle in response to fluctuating hormone levels. Estrogen dominance during the follicular phase promotes tissue thickening and increased discharge, while progesterone influence during the luteal phase may reduce lubrication and slightly alter pH.
Pregnancy Adaptations
During pregnancy, increased estrogen and progesterone levels cause vaginal tissues to become more vascular, softer, and more elastic in preparation for childbirth. These changes also increase vaginal discharge and may alter susceptibility to certain infections.
Menopause and Aging
Declining estrogen levels during menopause lead to vaginal atrophy, characterized by thinning tissues, decreased lubrication, loss of elasticity, and pH changes that can cause discomfort, pain during intercourse, and increased infection risk. These changes can significantly impact quality of life and sexual function.
Sexual Function and Response
Arousal Response
Sexual arousal triggers a complex cascade of vascular, muscular, and glandular changes in the vagina including vasocongestion (increased blood flow), vaginal tenting and lengthening, lubrication production, and increased sensitivity to stimulation. These changes optimize the vaginal environment for sexual activity.
Lubrication Mechanisms
Vaginal lubrication occurs through multiple mechanisms including transudation (fluid seeping through vaginal walls), secretions from Bartholin’s glands and other structures, and cervical mucus production. Adequate lubrication is essential for comfortable sexual activity and prevention of tissue trauma.
Orgasmic Response
During orgasm, the vagina experiences rhythmic contractions of the surrounding muscles, increased blood flow, and intense sensations. The vaginal response is part of the broader pelvic orgasmic response involving multiple anatomical structures and neural pathways.
Individual Variation in Response
Sexual response patterns vary significantly among women due to anatomical differences, hormonal factors, psychological states, relationship factors, and life experiences. Understanding this variation helps normalize diverse sexual experiences and identify when professional consultation may be beneficial.
Common Vaginal Conditions
Bacterial Vaginosis
Bacterial vaginosis is the most common vaginal infection, characterized by overgrowth of harmful bacteria and reduction in protective Lactobacillus species. Symptoms include thin, grayish discharge with a fishy odor, though many cases are asymptomatic. Treatment typically involves antibiotics to restore bacterial balance.
Vulvovaginal Candidiasis
Yeast infections, primarily caused by Candida albicans, affect up to 75% of women at least once. Symptoms include thick, white discharge, itching, burning, and irritation. Risk factors include antibiotic use, diabetes, pregnancy, and immunosuppression.
Sexually Transmitted Infections
Various STIs can affect the vagina including chlamydia, gonorrhea, trichomoniasis, herpes, and HPV. These infections may cause discharge, irritation, pain, or be asymptomatic. Regular screening and safe sexual practices are important preventive measures.
Vaginal Atrophy
Estrogen deficiency, particularly after menopause, can cause vaginal atrophy with symptoms including dryness, burning, painful intercourse, and urinary symptoms. Treatment options include topical estrogen, moisturizers, lubricants, and lifestyle modifications.
Hygiene and Care
Normal Hygiene Practices
Appropriate vaginal hygiene involves gentle external cleaning with mild soap and water, avoiding douching or harsh chemicals, wearing breathable cotton underwear, and changing tampons or pads regularly during menstruation. The vagina’s self-cleaning mechanisms generally don’t require internal cleansing.
Harmful Practices to Avoid
Practices that can disrupt vaginal health include douching, using scented feminine products, wearing tight non-breathable clothing for extended periods, and using harsh soaps or antiseptics in the vaginal area. These practices can disrupt the natural microbiome and increase infection risk.
Menstrual Hygiene
Proper menstrual hygiene involves regular changing of menstrual products, choosing appropriate absorbency levels, and maintaining general cleanliness during menstruation. Various menstrual products (pads, tampons, cups) have different considerations for vaginal health.
Sexual Hygiene
Sexual hygiene practices that support vaginal health include urinating after sexual activity, using appropriate lubrication when needed, communicating with partners about cleanliness, and seeking prompt treatment for any concerning symptoms after sexual activity.
Developmental Changes
Childhood and Prepubertal Development
Before puberty, the vagina is shorter and narrower with thin epithelium and neutral pH due to low estrogen levels. The prepubertal vaginal environment is more susceptible to certain infections and irritations, requiring different care approaches than adult vaginal health.
Pubertal Changes
Puberty brings dramatic changes including vaginal lengthening and widening, epithelial thickening, pH acidification, and beginning of normal vaginal discharge. These changes reflect increasing estrogen production and mark the transition to adult reproductive capability.
Reproductive Years
During the reproductive years, the vagina maintains optimal structure and function under normal hormonal influences. This period typically involves regular menstrual cycles, potential pregnancies, and generally stable vaginal health with cyclical variations related to hormone fluctuations.
Postmenopausal Changes
After menopause, declining estrogen causes gradual vaginal changes including tissue thinning, decreased elasticity, reduced lubrication, and pH changes. These changes can affect sexual function and comfort, though various treatments can help maintain vaginal health and function.
Cultural and Social Aspects
Cultural Attitudes and Taboos
Cultural attitudes toward vaginal health vary significantly worldwide, with some cultures maintaining open discussions about women’s health while others consider vaginal topics taboo. These cultural factors can significantly influence healthcare-seeking behavior, health education effectiveness, and treatment compliance.
Education and Awareness
Comprehensive education about vaginal anatomy, normal function, and health maintenance is crucial for promoting women’s health. Educational initiatives help dispel myths, reduce shame and anxiety, and encourage appropriate healthcare utilization when problems arise.
Healthcare Access and Quality
Access to quality gynecological care varies significantly by geographic location, socioeconomic status, and cultural factors. Improving access to culturally sensitive, evidence-based vaginal health care is an important public health goal.
Feminist Health Perspectives
The women’s health movement has emphasized the importance of women understanding their own bodies, including vaginal anatomy and function. Women’s health advocacy continues promoting body literacy, healthcare access, and research addressing women’s specific health needs.
Medical Evaluation and Care
Routine Gynecological Examinations
Regular gynecological examinations include visual inspection of external genitalia, speculum examination of the vagina and cervix, and sometimes internal palpation. These examinations help detect normal variations, identify problems early, and provide opportunities for health education and counseling.
Diagnostic Procedures
When problems arise, diagnostic procedures may include vaginal pH testing, microscopic examination of vaginal discharge, bacterial cultures, STI testing, and sometimes imaging studies or biopsies to evaluate specific conditions.
Treatment Approaches
Treatment for vaginal conditions depends on the specific diagnosis and may include antibiotics, antifungals, hormonal therapies, topical medications, or lifestyle modifications. Some conditions require ongoing management rather than one-time treatment.
Preventive Care
Preventive vaginal health care includes regular screening for infections and cancer, vaccination against HPV when appropriate, education about normal anatomy and function, and counseling about risk reduction strategies for various vaginal health problems.
Research and Future Directions
Microbiome Research
Ongoing research into the vaginal microbiome is revealing new insights into health and disease mechanisms, potential therapeutic targets, and personalized approaches to maintaining vaginal health. Probiotic therapies and microbiome-based treatments are areas of active investigation.
Hormonal Therapies
Research continues developing new hormonal treatments for menopausal vaginal symptoms, including novel delivery systems, selective estrogen receptor modulators, and combination therapies that optimize benefits while minimizing risks.
Regenerative Medicine
Emerging therapies including stem cell treatments, tissue engineering approaches, and regenerative medicine techniques may offer new options for treating vaginal atrophy, scarring, and other structural problems.
Personalized Medicine
Future approaches may include genetic testing to predict individual susceptibility to vaginal problems, personalized probiotic therapies based on individual microbiome characteristics, and customized treatment protocols based on individual anatomy and physiology.
Frequently Asked Questions
What is normal vaginal discharge?
Normal vaginal discharge varies throughout the menstrual cycle but is typically clear or white, mild-smelling, and doesn’t cause itching or burning. The amount and consistency change with hormonal fluctuations, increasing around ovulation and sometimes before menstruation. Concerning changes include strong odor, unusual color, or associated symptoms.
How should I clean my vagina?
The vagina is self-cleaning and only the external vulvar area needs gentle washing with mild soap and water. Avoid douching, scented products, or harsh chemicals inside the vagina, as these can disrupt the natural bacterial balance and increase infection risk.
Is it normal for vaginal size to vary?
Yes, significant individual variation in vaginal size, shape, and characteristics is completely normal. The vagina also changes size during arousal, expanding to accommodate sexual activity. These variations typically don’t affect function or health.
When should I see a doctor about vaginal symptoms?
Consult a healthcare provider for symptoms including unusual discharge (especially with strong odor), persistent itching or burning, pain during intercourse, unexplained bleeding, or any symptoms that concern you or interfere with daily life.
Can probiotics help vaginal health?
Some research suggests that certain probiotics may help maintain vaginal health by supporting beneficial bacteria, though evidence is still developing. Oral and vaginal probiotic preparations are available, but it’s best to discuss their use with a healthcare provider.
How does menopause affect vaginal health?
Menopause-related estrogen decline can cause vaginal dryness, thinning tissues, decreased elasticity, and pH changes. These changes can affect sexual comfort and increase infection risk, but various treatments including hormonal and non-hormonal options can help manage symptoms.
Are vaginal infections always sexually transmitted?
No, many vaginal infections like bacterial vaginosis and yeast infections are not sexually transmitted, though they can sometimes be triggered by sexual activity. However, some vaginal infections are STIs, so it’s important to get proper diagnosis and treatment when symptoms occur.